Pediatric Dentist Frisco Texas – Caring & Trusted!
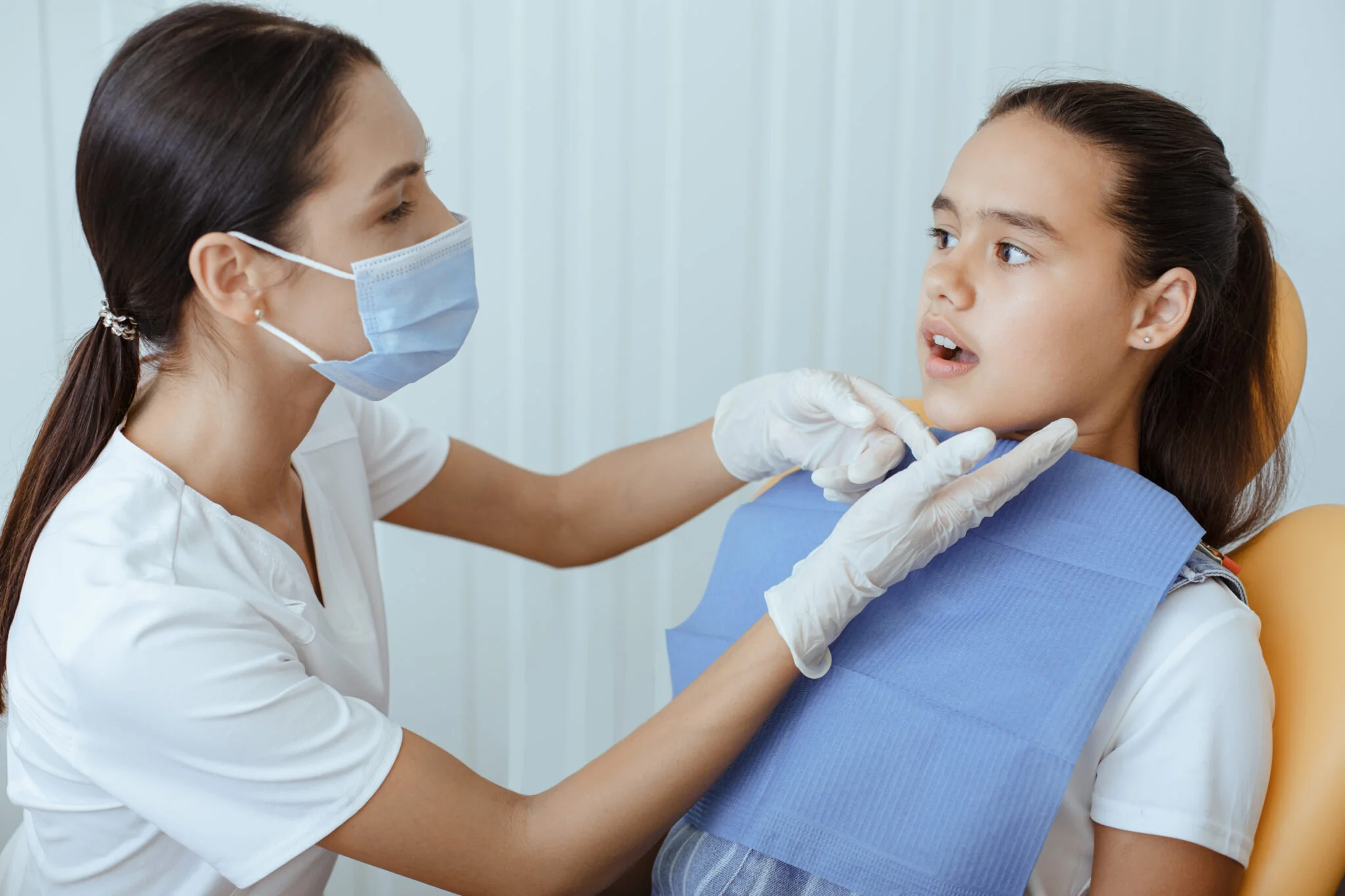
Sheer Smiles Kids is a Pediatric Dentist in Frisco Texas which aims to provide the highest level of pediatric dental care for kids of all ages—whatever their needs—in a fun, positive, and safe environment.
As a service to our New Patients, we provide you with the forms you need ahead of time so that we can help minimize your wait
We provide parental information and resources that provide our parents with the proper information for infants, toddlers, teens and children with special needs.
Dental services for your child should be a fun, safe and comfortable visit at the dentist.
About our Pediatric Dentist in Frisco Texas
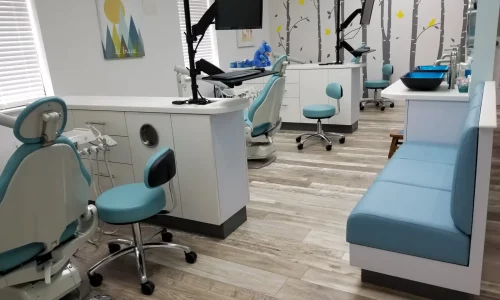
Your child will have a comfortable visit at our pediatric dental office located conveniently in heart of Frisco Texas.
Your child’s health is important. Therefore, our clinic provides the most advanced pediatric dentistry where our professionals will relax and entertain your child to ensure they have a great visit to the dentist every time.
Inspired by our beautiful home state of Texas, we foster health, wellness, and a sense of adventure in every child who comes through our doors. From the dental chair to the walking to school, we value meaningful interactions, quality care, and the pursuit of wellbeing.
Our focus is on dental prevention
We educate patients and parents on how oral hygiene and diet can affect the health of the child. We have a caring approach and dental and pediatric dentistry services you need. Remember, prevention is cheaper than treatment!
Has your child ever begged you not to leave the dentist? Impossible you say? Not at our office. It could be our gentle touch and a special way with kids. Our pediatric specialist and staff love children and are specially trained to put them at ease. At Sheer Smiles Pediatric Dentist Frisco Texas, we teach your children the proper way to take care of their teeth and just as important, they learn that going to the dentist can be fun.
It’s important for you and your children to feel comfortable when visiting the dentist and we make this our top priority.
In addition, at your Pediatric Dentist Frisco Texas we provide a fun environment where patients are worry-free. Thus, we know that one of the most important aspects of children’s dentistry is education.
We commit to offering treatment that meets or exceeds the guidelines and policies. Finally, Sheer Smiles pediatric dentist care for infants and children, including mentally challenged children. Come see us and learn what a difference a pediatric dentist specialist makes!
In short, Dr. Shir, your Pediatric Dentist Frisco Texas takes the time to talk to children on how to care for their teeth and gums. We emphasize the importance of good dental hygiene in preventing future treatments. Dr. Shir is board-certified by the American Board of Pediatric Dentistry.
Dr. Shir is a board certified pediatric dentists. From infants, toddlers, and preschoolers all the way up to adolescents, our experienced team remains committed to providing high quality and compassionate dental care for children of all ages. To learn more About Dr. Shir, DDS, or to request an appointment, please contact us here or call our office directly at (972) 987-0787.
Going to the dentist can be fun! Choose Sheer Smiles Kids to be your child's Pediatric Dentist!
About Dr. Solmaz Shir, DDS
Presently, Dr. Solmaz Shir is a Board Certified Specialist in Pediatric Dentistry. In addition, Dr. Shir, Received her Bachelor of Science in Clinical Laboratory Science from the University of Texas at Austin, and her Doctor of Dental Surgery (D.D.S) degree from University of Texas Health Science Center in San Antonio.
Specifically, Dr. Solmaz Shir graduated from dental school with a distinction in academic teaching. After that, she received numerous leadership, academic, and dentistry awards. As a result, Dr. Solmaz Shir has held a position as part-time faculty at Baylor College of Dentistry while practicing general dentistry in private practice setting in DFW area.

Sheer Smiles participates with most PPO insurance plans. Medicaid and CHIP accepted.















No Dental Insurance???
Our plan is designed to provide greater access to quality
dental care at an affordable price.

- Yearly maximums. None!
- Deductibles. Whats that?
- Claim forms. Nope!
- Frequency limits? None!
- No pre-authorization requirements.
- Pre-existing condition limitations. None!
- No one will be denied coverage.
- No waiting periods (immediate eligibility).
- For more details about what the plan includes, visit our Sheer Smiles VIP page
Same Day Pediatric Emergency Appointments!
Sudden dental injuries or severe pain can be frightening. In these emergency situations, we will be there to help your child, 24/7/365!


















What Our Kids Parents Think About Us!
Dr. Shir was amazing!!
Best pediatric dental I have visited!
My two little ones love going to Sheer Smiles!
Dr. Shir will provide the best Pediatric Dentistry services for your child!


What diet and nutritional advice can be offered for building strong teeth?
Experts agree that children need food from all the major food groups to grow properly and stay healthy. Too many carbohydrates, sugars (for example, from cake, cookies, candies, milk, fruit juice, and other sugary foods and beverages), and savory foods and starches (for example, pretzels and potato chips) can cause tooth decay. How long carbohydrates remain on the teeth is the main culprit that leads to tooth decay. Read more
The effects of fruit on kids teeth
We all know that fruit is full of vitamins and an important part of kids diets. But did you know that too much fruit (whether it’s fresh fruit, fruit juices, dried fruit or canned fruit) can have a negative effect and contribute to problems such as cavities and erosion, especially if your kids are grazing on fruit all day? Read more